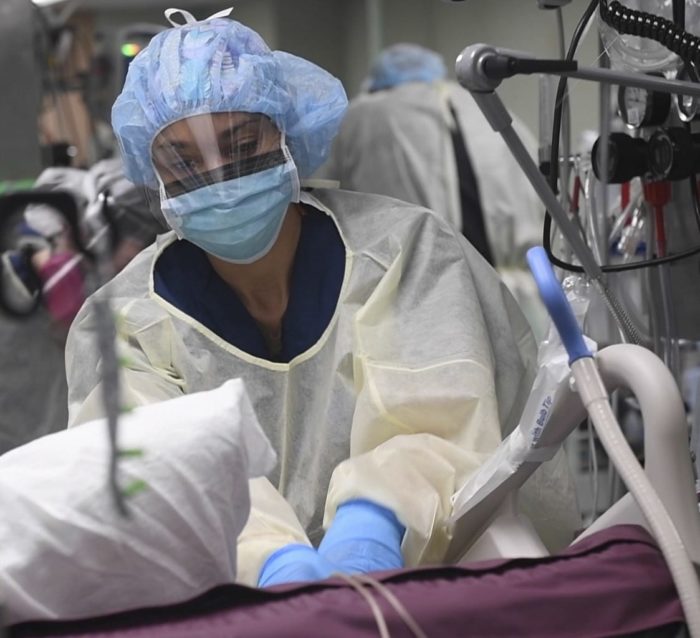
“Nursing homes that were given a clean bill of health and scored as satisfactory or exemplary in quality, staffing, and safety audits prior to the pandemic roundly failed in the face of crisis—a crisis that infectious disease scientists have predicted for years.”
The never-ending coronavirus news cycle had left me numb. By June I was sure that nothing further could surprise me about the mismanagement of the pandemic. I was mistaken. The Massachusetts Department of Health numbers on COVID-19 deaths at long-term care facilities (LTCFs) in the Commonwealth shocked me out of my stupor.
Scrolling through the tidy table of nursing homes and their COVID-19 infection and death counts in the state’s weekly coronavirus “dashboard,” I felt queasy. A few quick calculations revealed that dozens of LTCFs saw a quarter or more of their residents die from COVID-19 between March and June.
Like every Mass resident, I knew that nursing homes were struggling and that healthcare workers everywhere were experiencing a shortage of personal protective equipment. I had heard about how the National Guard was conducting mobile testing, and read stories about the Holyoke Soldiers’ Home, where at least a hundred veterans had died of the virus thanks in large part to gross negligence on the part of management. But I hadn’t grasped the scale of the crisis.
Long-term care facility deaths accounted for the majority of COVID-19 deaths in nearly every county in the state. In the Commonwealth, more than six out of 10 COVID-19 deaths occurred in LTCFs.
How did this happen? I wanted answers.
The DPH provided a detailed death count, so I assumed someone had already done a forensic analysis of what went wrong in the Commonwealth. Digging around, I found many good articles by local journalists detailing the heartbreak and fear of families and pointing to clues about why nursing homes were struggling. There were also a couple of national studies of nursing homes conducted by scholars at Harvard and the University of Chicago that suggested potential explanations.
But there was no detailed analysis of COVID-19 deaths in Massachusetts nursing homes—no satisfactory explanation for why such a wealthy, capable state had failed so badly at protecting its most vulnerable residents.
I enlisted the help of Pankaj Mehta, a physicist at Boston University who also happens to be my husband, to dig into the data. We took the DPH data and combined it with official Medicare provider data, census data, health disparity data, facility-level data on race and ethnicity, pricing data that we scraped from the web, and data on the Mass Executive Office of Health and Human Services’s isolation unit policy.
This data, we believed, would help us begin to understand why the coronavirus pandemic had so quickly and thoroughly overwhelmed long-term care facilities across the Commonwealth.
To be clear, Massachusetts isn’t alone in the failure of its nursing homes. According to the Foundation for Research on Equal Opportunity, approximately 45% of all COVID-19 deaths in the United States were residents in assisted living facilities and LTCFs.
In Mass, we counted at least 51 LTCFs that saw 20% or more of their residents die from COVID-19. In many nursing homes, COVID-19 deaths were 10, 15, or 20 times greater than the COVID-19 death rate for all Commonwealth residents aged 80 to 89 (as of June 17).
Our analysis also revealed that nursing homes that created “isolation units” to care for COVID-19 positive patients from hospitals, acute care centers, and elsewhere in exchange for supplemental payments from MassHealth suffered higher death rates than homes that did not establish isolation units. We don’t have proof that the isolation units were the cause of higher death rates in these facilities; it’s possible that higher COVID-19 death rates at these facilities were an artifact of COVID-19 positive patients that were brought in from elsewhere dying in the nursing home isolation units, thus increasing the overall death rates of those LTCFs. Nonetheless, the connection is deeply troubling, potentially underscoring the lunacy of putting COVID-19 positive patients in facilities housing the population most vulnerable to this highly contagious virus.
As of early August, the isolation unit policy remained in place, making further investigation of why these LTCFs had higher death rates absolutely essential.
On the whole, however, my quest for an explanation for why nursing homes in a wealthy, capable state were unable to protect their residents was a failure. We found a few weak correlations between death rates and facility size, ownership structure, and racial makeup, but no “smoking gun.”
Sifting through mountains of quantitative data, plotting dozens of relationships, revealed in stark relief the inadequacy of our existing tools to measure resilience in the nursing home sector. Existing quantitative data, collected at great effort and expense by state and federal officials, failed to provide an accurate measure of institutional resilience.
Nursing homes that were given a clean bill of health and scored as satisfactory or exemplary in quality, staffing, and safety audits prior to the pandemic roundly failed in the face of crisis—a crisis that infectious disease scientists have predicted for years.
I don’t consider our analysis to be a waste of time, however. Nor is the correct conclusion that there was nothing that could have been done to prevent the tragic wave of nursing home deaths.
Instead, the dearth of easy answers underscores how important it is for experts and advocates to dig deeper—to marshal the resources of the Commonwealth to figure out what happened, because the battle to quell the coronavirus pandemic is far from over.
Scientists say that the coronavirus, like HIV and influenza, could linger, causing death and disruption until a vaccine is developed, or the population reaches herd immunity. Moreover, infectious disease experts say coronaviruses and other infectious diseases with the potential to become pandemics are on the rise globally.
But the time for discovery is rapidly slipping through our fingers. The longer we wait to reckon with nursing home failures and systematically assess what went wrong with a team of dedicated, on-the-ground researchers, the less likely we’ll be able to develop an effective plan to protect our state’s least resilient residents.
A full copy of the report can be found here and a long form feature on the study here. BINJ will continue to investigate the nursing home crisis in Massachusetts and will publish a follow-up study examining how we can protect our state’s most vulnerable residents.
Nicole is a writer, editor, and public sociologist. Nicole is the author of The New Prophets of Capital and The Smartphone Society, and is a staff writer at Jacobin magazine and managing editor at the Boston Institute for Nonprofit Journalism. She received her Ph.D. in sociology from Johns Hopkins University and previously taught at Boston University.

